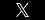Medically induced cooling of the brain can help treat damage. This relatively new procedure — the FDA approved it a little over 10 years ago — provides the opportunity to treat babies who are suffering from hypoxic brain damage because of perinatal asphyxia.
We don’t totally understand the exact science of why brain cooling limits birth injuries. Many theories make perfect sense floating around. But, ultimately, who cares why it works? It appears to work on not only the brain but other vital organs that have been harmed by oxygen deprivation.
At this point, I don’t know why any hospital with a NICU would not be capable of using cooling to protect an infant from brain damage.
How does cooling therapy work?
Cooling therapy uses a purpose-made cap, a special blanket, or a mattress to cool the newborn at a controlled temperature. It can be used to cool either the baby’s head or their entire body.
Medical professionals apply cooling therapy according to the severity of the infant’s injuries. More severe injuries need longer durations of cooling therapy. Cooling therapy can last for two to three days.
What is hypoxic-ischemic brain damage, and how is it related to birth-related injuries?
Hypoxic brain damage occurs when the brain is not getting enough oxygen. The term hypoxia means a deficiency in the amount of oxygen reaching the tissues. It contrasts with anoxic brain damage, which means there is no supply of oxygen to the brain.
Hypoxia at birth is known as hypoxic-ischemic encephalopathy (HIE). It is also known as perinatal asphyxia. HIE can be caused by different factors. They include trauma to the infant in utero, placental problems, an umbilical cord prolapse, preeclampsia, eclampsia, overmedication of the mother, or shoulder dystocia. It usually occurs around the time of birth and can cause death in about 25 to 50 percent of severe cases.
What is brain cooling and how does it work?
Therapeutic hypothermia, also known as brain cooling, is a process where the body temperature is reduced to a norm.
How does head cooling work for a brain injury? Head cooling drops the metabolic rate of the brain. This alters the release of cytokines.
What are cytokines?
Cytokines are chemical mediators of inflammation. The research is clear that pro-inflammatory mediators of the cytokine family are highly associated and lead to brain injury following infection.
Brain Cooling and Cerebral Edema
Brain cooling also relieves pressure in the brain caused by cerebral edema. Cooling therapy is thought to reduce energy depletion and decrease transmitter activity in the brain. Cooling therapy can also reduce ion flux alterations. Whatever the mechanism, and we don’t fully understand it completely yet, postnatal cooling of the brain has a beneficial effect on the outcome.
What happens after cooling therapy?
After cooling therapy, doctors provide assessments and monitoring to make sure they can function healthily. Professionals will provide further tests such as MRIs, EEGs, and heart monitors. This is done to detect possible abnormal brain, electrical, or heart activity.
What test indicates perinatal asphyxia?
If the child has an arterial cord blood gas score that below 7.1, the child is through to have perinatal asphyxia. Some doctors and ACOG have suggested 7.0 or lower and an APGAR of below 4. But a 7.1 or lower blood gas is the more common threshold.
What is the criteria to initiate cooling for a child who may have brain damage?
The standard often used to initiate cooling therapy is if the pH is less than 7 or base excess is greater than 16 before 60 minutes of birth (yes, this is a little bit of pushback on my last answer of a pH level of 7.1 as the standard).
There are several other things that doctors may consider to determine whether a baby for brain cooling. They may look at Apgar scores and require a score of less than 5 after 10 minutes of birth. (The Apgar score is a test that determines a newborn child’s health in relation to infant mortality. It checks skin color, pulse rate, reflex irritability grimace, activity, and respiratory effort.)
Other criteria may include whether the child:
- needs resuscitation and oxygen after ten minutes of birth
- was born within 36 weeks of gestation or more
- is thought to have moderate-to-severe encephalopathy
University of Edinburgh study
Researchers from the University of Edinburgh conducted a study on medical induced cooling effects on the brain and head-related injuries. Engineers and medical experts at the university collaborated to create a 3D model of the brain. This model considered simultaneous flow, heat transfer, and metabolism between arteries, veins, and brain tissue in three dimensions throughout the brain.
Through computer simulations, researchers discovered that cooling newborn babies’ heads to 10°C (50°F) would allow their core brain temperature to fall from 37°C to 36°C (98.6°F to 96.8°F). This temperature is low enough to help recovery. Researchers say that this could help babies at risk of long-term damage from birth complications.
The take home message is that cooling can prompt a beneficial drop in temperature deep in the brain, which can relieve pressure inside the head and prevent further injury. Cooling could also be used to aid newborn babies at risk of long-term damage from birth complications without cooling their entire body.
Oxford University and Imperial College study
An Oxford University and Imperial College London study looked at how brain cooling can treat perinatal hypoxia. It was named the Total Body Hypothermia for Neonatal Encephalopathy Trial (TOBY). The TOBY clinical trial involved 325 newborn babies who experienced hypoxia at birth. They were randomly assigned into two groups within six hours of delivery. One group was treated with standard care. The other group received both standard care and brain cooling. This group had their body temperature reduced to 33.5°C (92.3°F) for 72 hours. After 72 hours, they would be slowly returned to a normal body temperature of 37°C (98.6°F).
Researchers found that 51.7% of oxygen-deprived babies who were treated with brain cooling survived to age six to seven years with a normal IQ. Only 39.4% of babies who received standard care did the same. Brain cooling reduced the risk of cerebral palsy and other disabilities in children. However, there was no difference in mortality rate between standard care and brain cooling-treated groups. The mortality rate was about 30% for both groups.
Are there any risks associated with brain cooling?
Research suggests there are few risks associated with cooling therapy for children with hypoxia if done correctly. Trials seem to suggest there are more positive than negative benefits.
The most common side effect that appears to be a risk is sinus bradycardia, known as a slowed heart rate. However, it is not a life-threatening condition. It can also be treated depending on its cause and severity. The biggest risk of cooling therapy, it would seem, is not doing it at all or not doing it correctly.
Erythropoietin with Cooling Therapy
Erythropoietin, commonly known as EPO, is a hormone naturally produced by the kidneys that stimulates the production of red blood cells in the bone marrow. It plays a crucial role in regulating the amount of oxygen carried by the blood to the body’s tissues. In addition to its role in erythropoiesis, erythropoietin has been studied and used for its potential therapeutic benefits in various medical conditions, such as anemia, chronic kidney disease, and hypoxic ischemic encephalopathy in newborns.
In 2022, a study published in the New England Journal of Medicine pushed back on this hypothesis. This study found that adding erythropoietin to cooling therapy does not provide any additional benefits for term newborns with birth asphyxia, compared to cooling therapy alone. The study involved 500 infants with moderate or severe hypoxic ischemic encephalopathy and showed that both groups, one receiving hypothermia treatment only and the other receiving hypothermia plus erythropoietin, had an equal risk of death or neurodevelopmental impairment at 2 to 3 years of age. In fact, the erythropoietin group had more serious adverse events during the newborn period than the placebo group.
 Maryland Injury Law Center
Maryland Injury Law Center